Exercise¶
Hands-down, exercise is the most commonly discussed topic of long-term Loop users. Exercise is highly specific to an individual and its impact on blood sugar is not always equal. For example, many people find anaerobic exercise such as weight lifting will raise blood glucose (BG), and aerobic exercise such as running will lower BG. The degree to which impacts are observed also depends on the insulin and carbohydrates on board going into the exercise. Blood glucose response in competition can be quite different than a regular training session due to the added adrenaline. Exercising with T1D does require extra preparation, but with preparation, things should go much easier.
If you exercise consistently, you will figure out a pattern and can plan ahead.
If you are just starting an exercise progam, it will take time to become accustomed to the new routine. After your body is used to regular exercise, the impacts on your glucose and insulin regimen are likely to change again.
Loop-Specific Exercise Tips (Start Here!)¶
Key Strategy: Use Override Targets Ahead of Time¶
Reduce insulin on board (IOB) before exercise by setting an override with a higher target:
- When: Start 1-2 hours BEFORE exercise (not when you start)
- Target increase: Usually 50 mg/dL higher than normal (adjust based on your needs)
- Why: Loop needs time to decrease basal insulin before aerobic exercise begins
Example: If your normal target is 100 mg/dL, set an exercise override to 150 mg/dL.
After Exercise: Continue the Override¶
Insulin sensitivity stays elevated for up to 24 hours after exercise:
- Keep your override active for hours after you finish
- Duration depends on exercise intensity and length
- Prevents post-exercise lows from increased insulin sensitivity
See the Override Targets page for detailed instructions on setting up and using overrides.
Pre-Exercise Meal Timing¶
- Minimize heavy carb meals in the 3 hours before intense exercise
- Large boluses create high IOB that increases low risk during exercise
- Consider partial boluses and slower, lower-carb snacks if eating beforehand
- Loop automatically recommends smaller boluses when override targets are active
Exercise Basics and Background¶
For more comprehensive background on exercise and Type 1 diabetes, JDRF's PEAK (T1D Performance in Exercise and Knowledge) education curriculum provides excellent resources (source), including this article about exercise and T1D for athletes).
Click to expand: Detailed JDRF Exercise Guidelines
With great exercise, comes great responsibility
It goes both ways: exercise affects glucose control; glucose control affects exercise. Consistent physical activity produces consistent insulin sensitivity, which helps the body process glucose more evenly (avoid spikes), maybe even improving HbA1c.
Some considerations:
- Risk for hypoglycemia can be reduced by avoiding too much insulin on board (IOB) during and after exercise.
- Continuous glucose monitors (CGMs) or regular blood glucose testing provides critical information to preemptively minimize blood-sugar highs and lows.
- Plan ahead! Reduce insulin and add carbs for aerobic (longer duration, lower intensity) exercise, which causes blood sugar to drop, or increase for anaerobic (short duration, high intensity), which may cause spikes.
- After most exercise, insulin sensitivity is higher for 24 hours. Carbohydrates needed to replace liver glycogen levels must be balanced with decreased insulin levels.
Intensity. Speed. Environment. Duration . . . all affect the body’s reaction
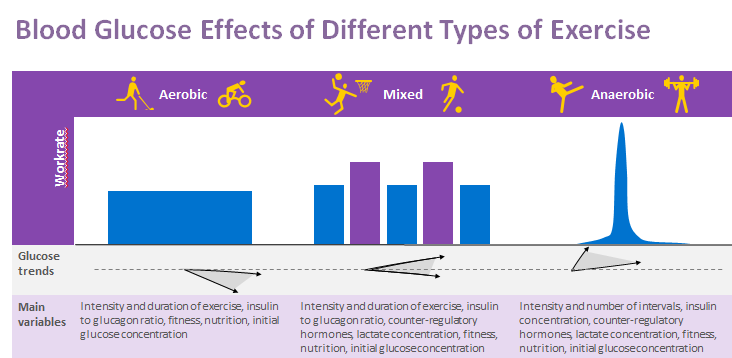
There are three types of exercise:
- Aerobic
- Aerobic exercise is usually continuous, light-to moderate intensity exercise and includes activities like running, walking, long-distance swimming, biking or tennis. Aerobic exercise typically tends to lower blood glucose levels.
- Anaerobic
- Anaerobic exercise is generally shorter in duration, of maximal to super max intensity and includes activities like sprinting, gymnastic, ice hockey, or weight training. Anaerobic exercise typically tends to raise blood glucose levels.
- Mixed
- Mixed exercise is combination of the aerobic and anaerobic activity such as basketball or soccer. Managing blood glucose levels with mixed exercise is difficult, but using a tool like a continuous glucose monitor can help greatly.
Glucose levels during sports affect performance in many ways: strength, stamina, speed, agility, flexibility, safety and mental sharpness.
- Insulin resistance, which is when the body requires more insulin to process glucose, is a problem. Exercise combats this by increasing insulin sensitivity and glucose uptake by muscles. Muscles are better able to absorb glucose when contracted.
- Exercise thwarts postprandial (after-meal) hyperglycemia by slowing carbohydrate absorption, increasing glucose utilization and accelerating insulin action.
- Practice vs game day – each can have dramatically different effects on your T1D. Adrenaline and stress both raise blood glucose levels and are typically present on the day of your game or event.
Balancing Act: Finding your blood glucose zone and peak fitness zone
Caution: Delayed Onset Hypoglycemia can occur 6 to 12 hours (sometimes 24 hours) after exhaustive exercise, due to replenishment of muscle glycogen stores and enhanced insulin sensitivity. It is possible to prevent this by:
- keeping records of your fitness regimen and the effects it has on your body
- using a CGM or frequent blood testing to monitor your body’s response to activity
- decreasing basal insulin or meal boluses after activity
- consuming slow-acting carbohydrates after activity
Similar recording and monitoring tactics can be used to prevent hyperglycemia (blood-sugar highs). Some other options include:
- bolusing (at a half dose) 30 to 60 minutes prior to activity to offset rise of blood glucose, delayed bolusing or adding post-workout cool-down (depending on conditions of rise)
- incorporating relaxation, breathing, visualization tools to address pre-workout emotional stress
- limiting pump disconnection time
- hydrating
- administering rapid-acting insulin (only under certain conditions)
Summary¶
Exercise with Loop requires planning ahead:
- Before: Set override target 1-2 hours early to reduce IOB
- During: Monitor CGM and adjust carbs/override as needed
- After: Keep override active to manage increased insulin sensitivity
- Depending on the type of exercise, how accustomed your body is to exercise, and whether the Insulin Needs setting is adjusted in the override - you may need to turn off the override when you stop the exercise
- Learn: Track what works for your specific exercise types and intensity levels